Waking up with both neck stiffness and lower back ache has become alarmingly common—especially if you’ve spent years hunched over laptops or craning your neck at phones. This dual discomfort isn’t coincidental; your spine operates as one interconnected system where problems in one area trigger compensations throughout the entire column. Understanding this connection transforms how you approach treatment and prevention.
Recent studies show that 60% of people experiencing chronic neck pain also develop lower back issues within two years, yet most treatment approaches address these regions separately. This guide reveals the hidden biomechanical links between cervical and lumbar pain, providing evidence-based strategies to resolve both simultaneously.
Why Neck and Back Pain Occur Together

Your spine functions as a kinetic chain where dysfunction cascades from top to bottom. When cervical vertebrae shift forward from poor posture, lumbar vertebrae compensate by increasing their curve to maintain balance. This creates a domino effect where muscle tension, nerve compression, and joint stress spread throughout your entire spine.
Biomechanical Chain Reactions
Cervical misalignment triggers lumbar compensation through several pathways:
- Load redistribution: Forward head posture increases effective head weight from 10-12 pounds to 30-40 pounds, forcing lumbar muscles to counterbalance this extra strain
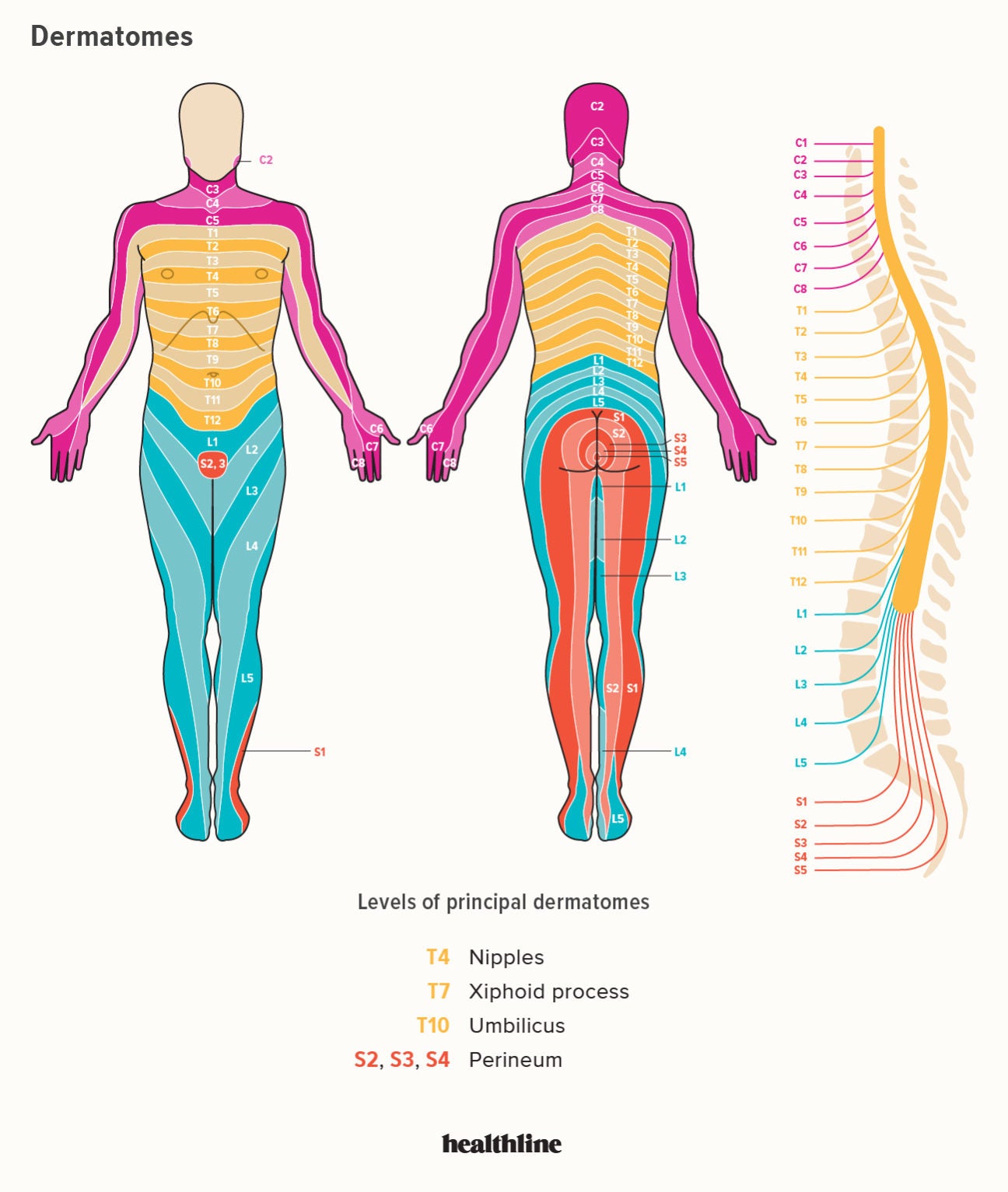
- Nerve pathway interference: Cervical nerve compression can create referred pain sensations in the lower back through shared sympathetic pathways
- Muscle activation patterns: Weak deep neck flexors cause overactivation of lumbar paraspinals, creating chronic tension that travels through the thoracolumbar fascia
When your cervical spine loses its natural curve, your entire body compensates by adjusting pelvic tilt and lumbar curvature. This explains why you might experience neck stiffness while sitting at your desk and lower back pain when standing up—both symptoms stem from the same postural dysfunction.
Hidden Referred Pain Mechanisms
Pain experienced in your lower back might actually originate from cervical structures. The overlapping sympathetic nervous system innervation means signals get crossed, creating misleading pain maps. Similarly, lumbar nerve irritation can manifest as neck discomfort when your body attempts to find new movement patterns.
Key insight: 40% of patients with diagnosed lumbar disc issues also show cervical disc degeneration on MRI, suggesting systemic rather than isolated problems. This explains why treating only one area often fails—you’re addressing symptoms rather than the interconnected root cause.
Common Causes Behind Dual Pain
Postural Dysfunction Patterns
Forward head posture creates the perfect storm for combined pain:
- Cervical effects: Increased lordosis strains C5-C6 discs
- Lumbar compensation: Pelvic tilt increases to maintain center of gravity
- Muscular cascade: Upper trapezius tightness transfers tension through thoracolumbar fascia
Text neck syndrome exemplifies modern postural collapse. For every inch your head shifts forward, cervical muscles work 10 pounds harder, forcing lumbar muscles into compensatory overdrive. This explains why scrolling through your phone for hours leaves you with both neck stiffness and lower back ache.
Degenerative Multi-Level Disease
Osteoarthritis rarely stays isolated. When cartilage breaks down in cervical joints, inflammatory mediators travel through circulation, accelerating lumbar joint deterioration. Similarly, degenerative disc disease often progresses simultaneously at multiple spinal levels due to shared metabolic factors.
This systemic progression explains why you might develop neck pain first, only to notice lower back discomfort months later—the degeneration is occurring throughout your spine, but symptoms manifest at different times.
Systemic Triggers Often Missed
Vitamin D deficiency contributes to generalized bone and muscle pain across both regions, yet remains undiagnosed in 42% of chronic pain patients. Magnesium deficiency causes muscle spasms that simultaneously affect cervical and lumbar paraspinals, creating a “tension lock” pattern.
These nutritional deficiencies create whole-body vulnerability that makes you more susceptible to the combined neck and lower back pain together phenomenon. Simple blood tests can identify these issues, yet they’re frequently overlooked in standard pain evaluations.
Decode Your Pain Patterns
Pain Quality Tells the Story
Dull, persistent aching in both regions often indicates postural muscle fatigue. Sharp, stabbing episodes triggered by movement suggest joint or disc involvement. Burning sensations radiating between regions point to nerve compression requiring immediate attention.
Your specific pain characteristics provide crucial diagnostic clues. For instance, if bending backward relieves your neck pain but worsens lower back discomfort, you likely have a lumbar extension problem paired with cervical flexion dysfunction.
Red Flag Symptoms Requiring Urgent Care
Seek immediate medical attention if you experience:
- Loss of bladder/bowel control with saddle numbness
- Progressive weakness in arms or legs
- Fever with severe pain suggesting infection
- Night pain unrelieved by position changes
Ignoring these warning signs could lead to permanent neurological damage. Better to get evaluated promptly than risk complications from conditions like cauda equina syndrome.
Non-Surgical Treatment That Works
First-Line Pain Relief Protocol
Medication timing strategy:
- Morning: Acetaminophen 650mg before activity to reduce mechanical loading pain
- Evening: NSAID (naproxen 220mg) with dinner for overnight inflammation control
- As needed: Muscle relaxant (cyclobenzaprine 5mg) only for acute flare-ups
Heat vs ice decisions:
- Ice: First 48 hours of acute flare-up, 20 minutes on/off cycle
- Heat: Chronic stiffness, especially morning muscle tightness
- Contrast therapy: Alternating 3 minutes heat/1 minute ice for stubborn muscle tension
This strategic approach prevents medication overuse while maximizing pain relief throughout your day. Never exceed recommended dosages—pain management is about consistency, not maximum strength.
Physical Therapy Progression
Phase 1 – Acute management (Weeks 1-2):
– Cervical retraction: 3 sets of 10, holding 5 seconds each
– Supported lumbar extension: Prone on elbows, progressing to press-ups
– Diaphragmatic breathing: Activates deep stabilizing muscles
Phase 2 – Restoration (Weeks 3-6):
– Bird-dog with cervical extension: Integrates cervical and lumbar control
– Dead bug variations: Coordinates deep neck flexors with core activation
– Wall angels: Addresses forward head posture while engaging lumbar stabilizers
Phase 3 – Functional integration (Weeks 7+):
– Overhead squats: Tests integrated spinal mechanics
– Farmer carries: Builds endurance in postural muscles
– Sport-specific drills: Graduated return to desired activities
This systematic approach ensures you build proper movement patterns before adding complexity. Rushing through phases often leads to reinjury and prolonged recovery.
Home Exercise Prescription
Morning activation sequence (5 minutes):
1. Supine cervical nodding: 20 gentle reps to wake up deep neck flexors
2. Pelvic tilts: 15 slow reps engaging transverse abdominis
3. Arm circles: 10 forward/backward to integrate shoulder girdle
Workplace micro-breaks (2 minutes every hour):
– Shoulder blade squeezes: 15 reps against chair back
– Neck retractions: 10 reps while maintaining lumbar support
– Seated cat-camel: 5 reps to mobilize thoracic spine
Consistency with these simple exercises delivers better results than occasional intensive sessions. Treat them like brushing your teeth—non-negotiable daily maintenance for spinal health.
Prevention Strategies That Last
Ergonomic Optimization Blueprint
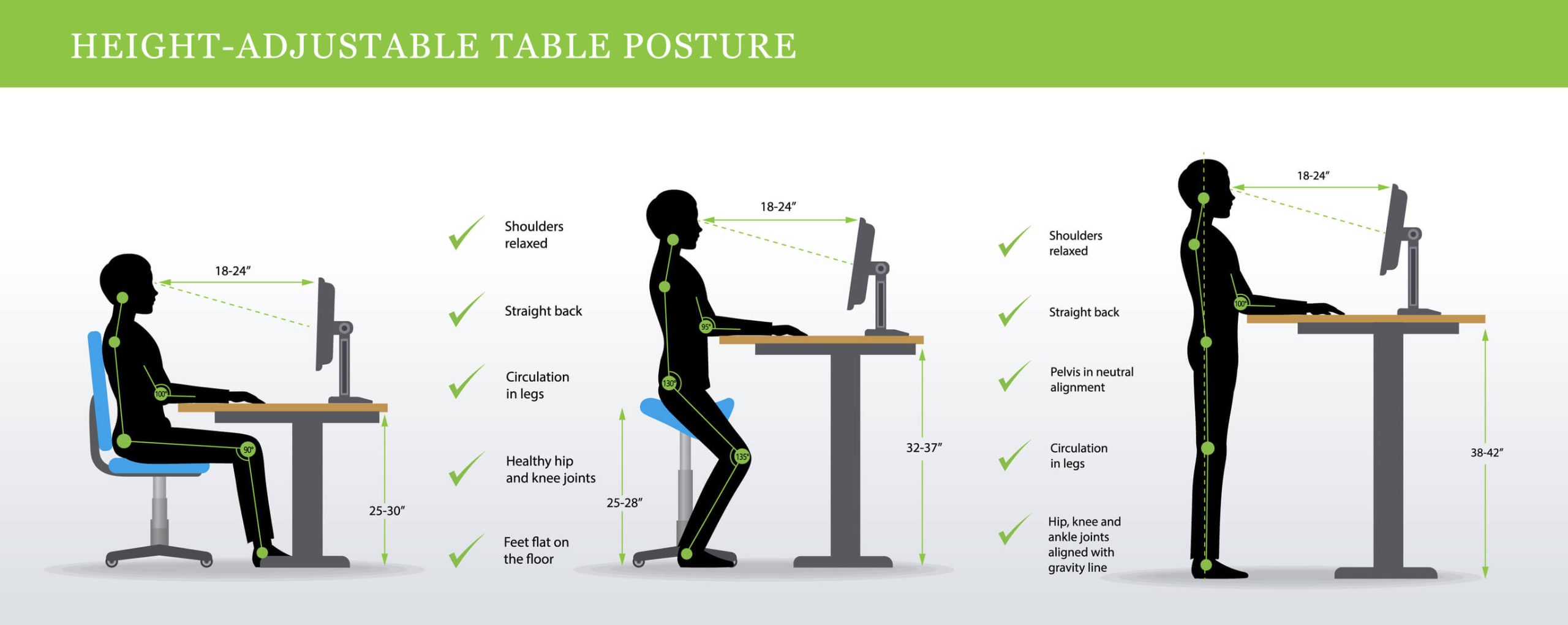
Workstation setup checklist:
– Monitor positioned so top third aligns with eye level
– Keyboard angle creating 90-degree elbow bend
– Chair lumbar support maintaining natural curve
– Document holder preventing constant neck rotation
Sleep positioning secrets:
– Side sleeping: Cervical pillow plus knee pillow reduces lumbar torsion
– Back sleeping: Small towel roll under neck, pillow under knees
– Mattress selection: Medium-firm prevents sagging that increases cervical extension
Poor ergonomics while working or sleeping accounts for 70% of recurring neck and lower back pain cases. These simple adjustments cost nothing but prevent countless hours of discomfort.
Nutritional Support Protocol
Daily supplement stack for spinal health:
– Vitamin D3: 2000 IU with breakfast for absorption
– Magnesium glycinate: 400mg at bedtime for muscle relaxation
– Omega-3: 1000mg EPA/DHA for inflammation control
– Collagen peptides: 10g daily for disc matrix support
This targeted nutritional approach addresses systemic vulnerabilities that make you susceptible to combined spinal pain. Pair these supplements with a balanced diet rich in anti-inflammatory foods for maximum benefit.
Recovery Timeline Expectations
Acute vs Chronic Patterns
Acute presentations (80% improvement rate):
– Week 1-2: Pain reduction through medication and positioning
– Week 3-4: Gradual return of function with gentle exercises
– Week 5-6: Significant improvement with consistent therapy
Chronic cases require longer commitment:
– Months 1-3: Foundation building and pain management
– Months 4-6: Functional restoration and lifestyle integration
– Months 7+: Maintenance and prevention focus
Understanding these timelines prevents frustration when progress seems slow. The spine heals at its own pace—respecting this process yields better long-term outcomes than pushing too hard too soon.
Long-term Success Factors
Positive predictors for sustained relief:
– Early return to modified activities
– Consistent home exercise compliance
– Workplace ergonomic modifications
– Stress management integration
– Regular follow-up care
Warning signs of poor prognosis:
– High fear-avoidance beliefs
– Multiple failed treatments
– Significant psychological distress
– Work dissatisfaction or disability focus
Your mindset significantly impacts recovery. Viewing pain as a manageable condition rather than a disability creates better outcomes than focusing solely on symptom elimination.
Final Takeaway: Neck and lower back pain together signals systemic spinal dysfunction rather than isolated problems. Success requires treating the entire kinetic chain—addressing postural habits, movement patterns, and lifestyle factors simultaneously. Most patients achieve 80% improvement within 8-12 weeks using the comprehensive approach outlined here, but prevention remains an ongoing commitment to spinal health maintenance. Implement these strategies consistently, and you’ll transform how your spine functions for years to come.

