If you’re searching “does scoliosis cause back pain,” you’re likely frustrated by contradictory information. The truth defies common sense: severe spinal curvature doesn’t automatically mean severe pain. Groundbreaking research reveals adolescents with 80° curves may experience minimal discomfort, while others with mild 25° curves suffer debilitating pain. This paradox explains why pain prevalence ranges from 23% to 90% across scoliosis populations – a 67-point spread that stunned researchers at Texas Scottish Rite Hospital when they found only 23% of 2,442 patients reported back pain, matching general population rates.
This confusion ends today. We’ll dissect exactly why your spine’s shape might not be the pain culprit, reveal the surprising factors that actually drive discomfort, and provide actionable steps for pain management based on the latest clinical evidence. You’ll learn to identify red flags requiring immediate attention and discover why psychological factors often outweigh curve severity in determining your pain experience.
Why Your Curve Size Doesn’t Determine Pain Intensity
Forget what you’ve been told about scoliosis pain. Multiple high-quality studies prove no correlation exists between Cobb angle measurements and pain intensity. A landmark analysis of 195 adolescent idiopathic scoliosis (AIS) patients with curves exceeding 30° found pain reports unrelated to curve magnitude. Even more startling: factors you’d assume matter – BMI, age at diagnosis, spinal alignment measurements – show zero relationship with pain levels.
Physical Factors That Actually Cause Scoliosis Pain
- Lumbar curve rigidity: Stiff curves correlate strongly with higher VAS pain scores
- Flattened thoracic spine: Reduced kyphosis increases mechanical stress on discs
- Pelvic asymmetry: Greater imbalance directly links to reported discomfort
- Family pain history: Genetic predisposition to nonspecific back pain amplifies risk
Psychological Drivers You Can’t Ignore
- Kinesiophobia: Fear of movement creates muscle tension that worsens pain
- Pain catastrophizing: Magnifying sensations increases disability by 40%
- Poor self-image: Lower SRS-22 scores in body image domains predict higher pain
- Anxiety/depression: Mental health status is twice as predictive as curve size
Pain Patterns That Reveal the Real Culprit
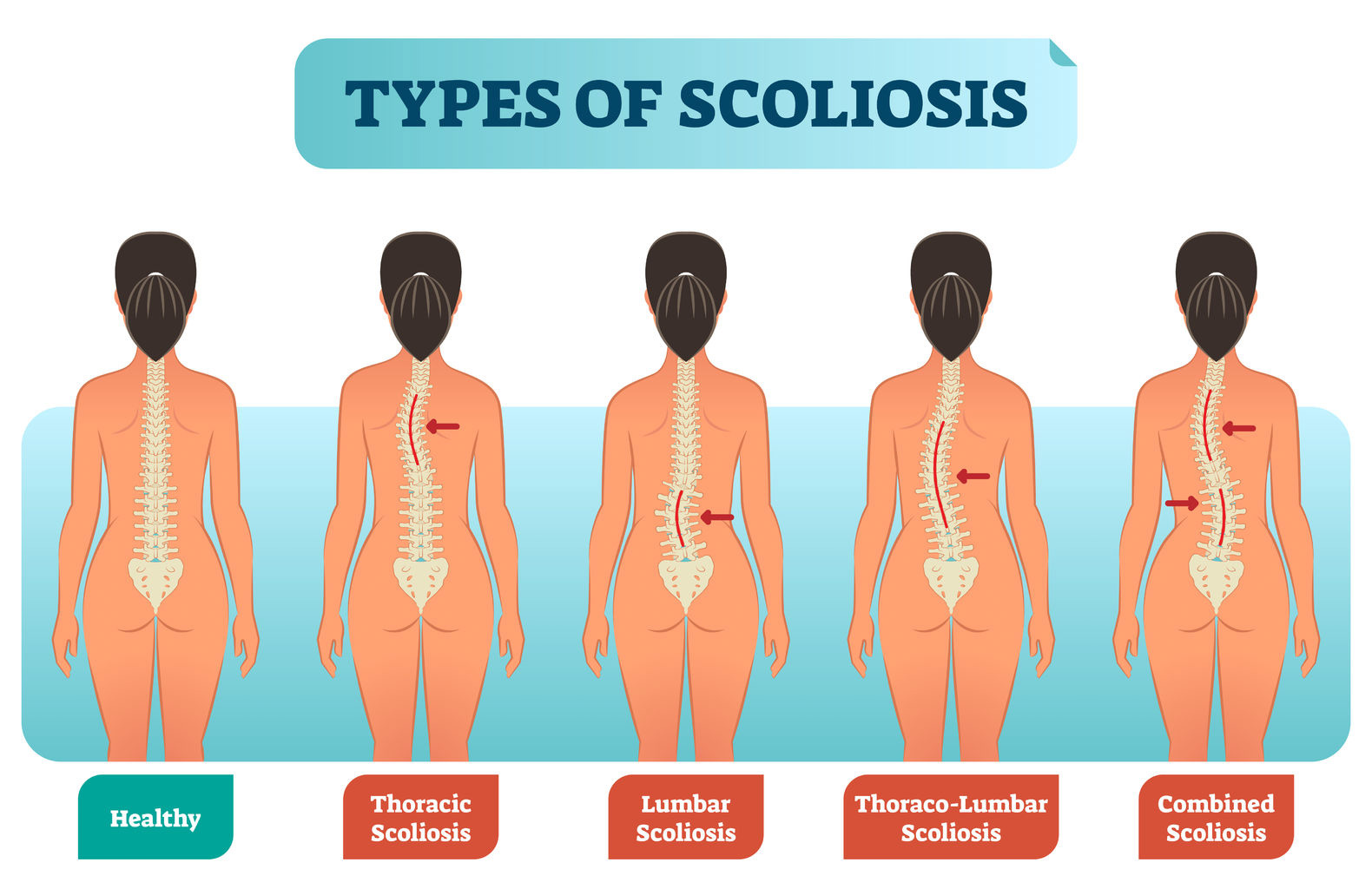
Your pain location tells a critical story. Upper right back pain dominates scoliosis cases (45% of reports), typically near the thoracic rib hump. This sharp, localized discomfort worsens with prolonged sitting and improves with position changes – a key differentiator from other back conditions. Meanwhile, lower back pain (17% of cases) often indicates mechanical stress from compensatory curves requiring disc evaluation.
Red Flag Symptoms Needing Immediate Evaluation
Don’t dismiss these warning signs as “just part of scoliosis”:
– Night pain disrupting sleep – rules out mechanical causes
– Progressive leg weakness – suggests neurological involvement
– Bowel/bladder changes – indicates possible cord compression
– Fever with spinal tenderness – signals potential infection
– Rapid curve progression with new pain – requires urgent MRI
Diagnostic Protocol for Painful Scoliosis

When pain accompanies scoliosis, “idiopathic” becomes a dangerous assumption. Painful AIS demands systematic evaluation to rule out underlying pathology. Clinics following best practices now implement this minimum assessment:
- Detailed pain mapping: Document location, triggers, and relieving factors
- Neurological screening: Test sensation, strength, and reflex changes
- Psychosocial assessment: Use Tampa Scale for kinesiophobia and PPST for risk stratification
- Family history review: Note chronic pain conditions alongside scoliosis
When to order MRI: If pain doesn’t match curve location, neurological symptoms appear, or red flags emerge. This is non-negotiable for reactive scoliosis where tumors or infections cause the curvature.
Proven Pain Management Strategies That Work
Forget one-size-fits-all approaches. Effective scoliosis pain relief requires targeting both physical and psychological drivers, as demonstrated in a recent multicenter study showing 68% pain reduction with combined therapies.
Physical Therapy That Actually Helps
- Core stabilization: Focus on deep abdominal muscles (transverse abdominis) and paraspinal stabilizers
- Concave-side stretching: Address tight muscles on the inner curve through targeted myofascial release
- Functional retraining: Practice proper lifting mechanics using the “hip hinge” technique
- Ergonomic modifications: Implement sit-stand desks with 30-minute position change intervals
Psychological Interventions with Clinical Proof
- Catastrophizing reduction: Cognitive restructuring to break “pain magnification” cycles
- Graded exposure: Systematically confront feared movements starting at 20% intensity
- Activity pacing: Use the “spoon theory” to balance energy expenditure
- Sleep optimization: Implement strict wind-down routines to improve pain thresholds
Surprising brace insight: Patients with brace treatment history report 32% lower pain scores – not from curve correction, but through improved postural awareness and core engagement.
Why Surgery Helps Pain (But Isn’t a Cure)

Spinal fusion primarily addresses curve progression, yet 70-80% of surgical patients report significant pain improvement. This occurs through:
– Correction of rigid curves causing mechanical stress
– Stabilization of unstable segments triggering pain
– Reduced muscle fatigue from compensatory patterns
Critical reality check: Chronic pain persists in 10-15% of fusion patients. Success depends on pre-op factors:
– Lower pre-surgical VAS scores predict better outcomes
– Psychological readiness (address anxiety/depression first)
– Realistic expectations (surgery isn’t primarily for pain)
Daily Prevention Tactics to Stop Pain Escalation
Adolescent pain patterns predict adult disability – making early intervention crucial. Implement these evidence-based strategies immediately:
Movement modifications that work:
– Change positions every 30 minutes (set phone reminders)
– Sleep with pillow support under knees for lumbar curves
– Choose swimming over running for cardiovascular exercise
– Use lumbar rolls in car seats during long drives
Pain monitoring system:
– Track daily VAS scores in a dedicated app
– Log activities triggering pain spikes (e.g., backpack use)
– Note mood correlations using a simple 1-5 scale
– Schedule curve checks every 6 months regardless of pain
Long-Term Outlook: Managing Pain Beyond Adolescence
The transition to adulthood requires strategic adjustments. Workplace ergonomics become critical – standing desks reduce pain by 41% compared to traditional seating. For women, pregnancy planning is essential as hormonal changes may destabilize curves. Most importantly, focus on functional metrics beyond pain scores:
- Activity tolerance: Measure sustained walking time (e.g., “I now walk 20 minutes without pain”)
- Medication reduction: Track decreasing reliance on NSAIDs
- Sleep quality: Aim for uninterrupted rest ≥6 hours nightly
- Quality of life: Monitor return to valued activities like dancing or hiking
Key Takeaway: The question “does scoliosis cause back pain” has no simple yes/no answer. While spinal curvature alone rarely generates pain, the combination of mechanical stressors, psychological factors, and individual susceptibility creates unique pain experiences. Success requires moving beyond curve measurements to address muscle imbalances, movement fears, and mental health – proven strategies that reduce pain by 68% when implemented early. Track your specific pain patterns, demand comprehensive evaluation when red flags appear, and remember: your curve size doesn’t dictate your pain destiny. With targeted interventions addressing both body and mind, most scoliosis patients achieve meaningful pain relief and maintain active lives.

