That satisfying post-workout burn can quickly turn into dread when your lower back starts screaming. Whether you’re a seasoned athlete or weekend warrior, lower back pain after exercise is frustratingly common—and often preventable. The good news? Most cases respond well to simple interventions you can do at home.
This guide walks you through everything you need to know: from distinguishing normal soreness from warning signs, to fixing the root causes, and building a bulletproof prevention plan. Stop guessing what’s wrong and start healing with these evidence-based strategies.
Pinpoint Your Lower Back Pain Type Within 24 Hours
Your lower back feels tight after deadlifts—should you panic or push through? Understanding the difference between healthy muscle adaptation and injury saves you weeks of frustration and unnecessary doctor visits.
DOMS Timeline: When to Relax vs. React
Delayed-onset muscle soreness (DOMS) is your body’s natural response to new or intense exercise. Here’s exactly what to expect with normal lower back pain after exercise:
- First 6–8 hours: Mild stiffness begins as your muscles react to unfamiliar stress
- 24–48 hours: Peak discomfort—achy, diffuse muscle tension that eases with movement
- 72 hours: Resolution—pain should steadily improve without intervention
The key difference? DOMS lives in the muscles, not the spine. You’ll feel tightness when stretching or contracting your core, but sharp pain when bending or twisting suggests something more serious.
Emergency Warning Signs You Can’t Ignore
Stop self-treatment immediately and seek professional help if you experience any of these red flags with your lower back pain after exercise:
- Sharp or shooting pain radiating down one or both legs
- Numbness or tingling in feet, legs, or groin area
- Progressive weakness—inability to stand on your toes or heels
- Loss of bladder or bowel control
- Fever above 101°F accompanying your back discomfort
- Pain lasting beyond 5 days despite rest and gentle stretching
These symptoms indicate potential nerve involvement or systemic issues requiring immediate medical evaluation.
Diagnose Your Specific Pain Cause
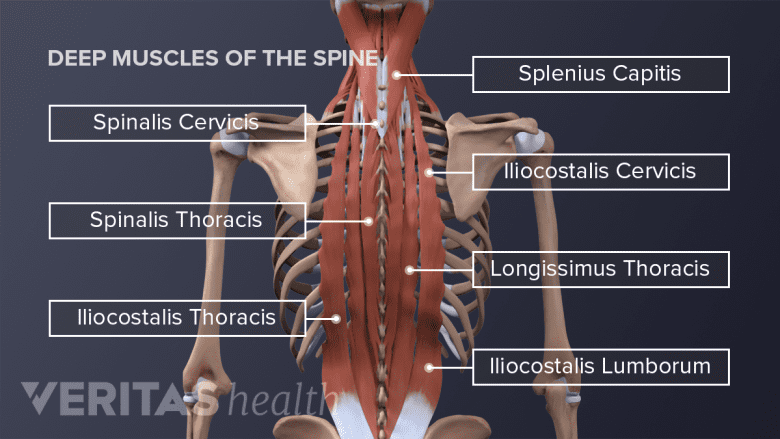
Lower back pain rarely has a single cause. Most cases involve a combination of mechanical stress, movement dysfunction, and recovery deficits. Identifying your specific trigger determines the right treatment approach.
Mechanical Stress Triggers
Lumbar strain represents the most common post-exercise back injury. Microscopic tears in muscle fibers create inflammation and protective spasms. Classic triggers include:
- Heavy deadlifts with rounded back creating excessive spinal loading
- Asymmetrical loads during single-arm carries or uneven squats
- Rapid progression in weight or volume without adequate adaptation
- Fatigue-induced form breakdown during final sets of compound movements
This type of lower back pain after exercise feels localized to one side, often with visible muscle spasms or tender knots you can feel with your fingers.
Movement Dysfunction Patterns
Your body compensates for weak links by overloading your lower back. Two common patterns create persistent pain:
Core weakness cascade:
– Transverse abdominis fails to stabilize your spine
– Erector spinae overwork to compensate
– Hip flexors tighten, pulling pelvis forward
– Result: excessive lumbar arch during squats and presses
Flexibility deficits creating stress:
– Tight hamstrings pull pelvis posteriorly
– Hip flexor tightness tilts pelvis anteriorly
– Both patterns force lumbar spine to compensate during movement
Immediate Treatment Protocol for First 72 Hours
The initial treatment phase determines your recovery trajectory. Aggressive early intervention often backfires—gentle movement combined with inflammation control works better than complete bed rest.
Step-by-Step Pain Reduction Plan
Days 1–2: Reduce inflammation
– Apply ice for 15 minutes every 2–3 hours (wrap in thin cloth)
– Take 200–400mg ibuprofen with food if medically appropriate
– Walk 5–10 minutes every waking hour—movement pumps nutrients to injured tissues
Day 3: Transition to heat
– Switch to 15-minute heat sessions to relax muscle spasms
– Begin gentle mobility: cat-camel, pelvic tilts, knee-to-chest stretches
– Avoid prolonged sitting—set a timer to stand every 30 minutes
Smart Movement Balance
Complete rest weakens supporting muscles and prolongs recovery. Instead, practice relative rest—avoid specific movements that trigger sharp pain while maintaining general activity.
Safe movements during acute phase:
– Cat-camel: On all fours, arch and round your back slowly
– Pelvic tilts: Lie on back, flatten lower spine into floor
– Gentle walking: Maintain natural arm swing, avoid hills
Avoid these pain triggers:
– Forward bends with straight legs
– Twisting movements
– Prolonged sitting or driving
– Heavy lifting or impact activities
Rebuild Strength Without Re-Injury

Once acute pain subsides (usually 3–7 days), progressive loading restores function and prevents recurrence. This phase requires patience—rushing back to heavy weights often re-injures healing tissues.
Foundational Core Activation
Start with these essential exercises, focusing on quality over quantity:
Dead Bug (3×10 each side)
– Lie on back, arms and legs in air
– Lower opposite arm/leg while maintaining back flat
– Progression: Add light resistance bands as pain allows
Bird-Dog (3×10 each side)
– On hands and knees, extend opposite arm and leg
– Hold 5 seconds, focus on preventing hip drop
– Regression: Start with arms only, then add legs
Glute Bridge (3×15 reps)
– Feet hip-width, knees bent
– Drive through heels, squeeze glutes
– Avoid arching lower back—focus on hip extension
Critical Flexibility Restoration
Tight muscles create compensatory movement patterns. Address these key areas daily:
Hamstring stretch (3×30 seconds each leg)
– Lie on back, strap around foot
– Keep knee slightly bent, pull leg toward chest
– Stop when you feel stretch, not pain
Hip flexor stretch (3×30 seconds each side)
– Half-kneeling lunge position
– Tuck pelvis under, reach overhead
– Hold onto chair for balance if needed
Prevent Future Lower Back Pain After Exercise
Prevention beats treatment every time. Build these habits into your training routine to stay pain-free.
Pre-Workout Activation Sequence
5-minute dynamic warm-up:
– Cardiovascular primer: 2 minutes jumping jacks or brisk walk
– Dynamic mobility:
– Leg swings: 10 each direction
– Hip circles: 10 each direction
– Cat-camel: 10 slow reps
– Bodyweight squats: 2×15 reps
Intra-Workout Technique Cues
Master these universal principles before adding weight:
Core bracing technique:
– Imagine preparing for a punch to the stomach
– Breathe normally while maintaining tension
– Practice during daily activities—brushing teeth, lifting groceries
Hip hinge pattern:
– Push hips back, not down
– Keep shins vertical, chest up
– Bar or weight stays close to body
– Drive through mid-foot, not toes
Load Management Strategy
10% rule for progression:
– Increase total weekly load (weight × reps × sets) by maximum 10%
– Example: If you lifted 10,000 lbs total last week, cap this week at 11,000 lbs
Deload weeks every 4–6 weeks:
– Reduce volume by 40–50%
– Focus on perfect form with lighter weights
– Use as technique practice, not vacation
Return to Exercise Without Setbacks
Rushing back too quickly creates the injury cycle. Follow this graduated approach based on pain-free function, not calendar days.
Phase-Based Progression
Phase 1 (Days 1–3): Foundation
– Pain-free range of motion achieved
– Body-weight movements only
– Walking, basic core activation
– Stop immediately if pain returns
Phase 2 (Days 4–7): Light resistance
– 30–40% of previous weights
– Perfect form focus—record yourself
– Single-leg balance work
– Monitor for 24-hour pain response
Phase 3 (Week 2): Progressive loading
– Gradual weight increases
– Compound movement patterns
– Pay attention to fatigue signs
– Maintain core activation throughout
Special Considerations for Your Situation
Different populations require modified approaches based on age, training history, and injury patterns.
Age-Related Adaptations
Under 40 years:
– Prioritize addressing mobility deficits
– Focus on correcting movement quality issues
– Consider previous injury history in your programming
40–60 years:
– Focus on core endurance over strength
– Account for potential degenerative changes
– Implement longer warm-up and recovery periods
Over 60 years:
– Consider osteoporosis precautions
– Avoid loaded spinal flexion movements
– Emphasize balance and stability work
Key Takeaways for Permanent Relief

Lower back pain after exercise is common but rarely serious. Most cases resolve within 6 weeks with proper management. Success hinges on:
- Early recognition of concerning symptoms versus normal soreness
- Adequate initial rest without complete immobilization
- Progressive strength rebuilding focusing on core and hip function
- Movement pattern correction to prevent recurrence
- Patient progression following pain-free milestones
Remember: temporary setbacks are opportunities to build resilience. Use this recovery period to address underlying weaknesses—you’ll return stronger and more knowledgeable than before. Implement these strategies consistently, and you’ll transform how your lower back responds to exercise permanently.

