That sharp ache in your lower back hits when you’re already fighting cancer. You’re sitting up in bed after your latest chemo infusion, and a burning sensation radiates from your spine down both legs. This isn’t just ordinary soreness—it’s chemotherapy-induced back pain affecting 57-83% of patients on taxane drugs. The good news? You can actively reduce this pain while continuing treatment. This guide delivers specific, doctor-approved strategies to ease your discomfort starting today.
Unlike typical back pain, chemo-related pain stems from nerve damage, inflammation, and bone marrow disruption caused by treatment. You’ll discover exactly why taxanes trigger burning sensations within 48 hours and how to stop misfiring nerves from sending false pain signals. Most importantly, you’ll learn which interventions work immediately versus those requiring medical coordination—so you can take control without compromising your cancer care.
Pinpoint Your Chemotherapy Back Pain Cause
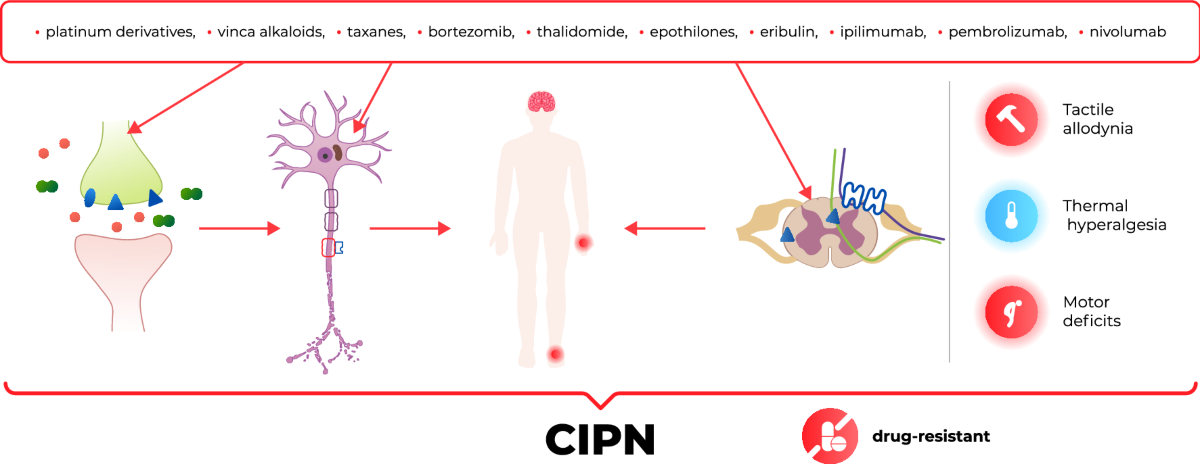
Nerve Damage Pathways Explained
Chemotherapy drugs like taxanes attack cancer cells but also damage your nervous system. This creates chemotherapy-induced peripheral neuropathy (CIPN), where damaged nerves send false pain signals to your brain. The process unfolds in three predictable stages:
- Immediate damage: Burning sensations begin within 24-48 hours of infusion
- Inflammatory response: Spinal tissues swell, adding mechanical pressure
- Neuropathic pain: Damaged nerves misfire continuously, causing chronic discomfort
You’ll recognize this as electric shock sensations shooting from your spine down both legs, often with tingling or numbness that worsens when walking. Symptoms typically emerge within your first two months of treatment and intensify with each cycle.
Three Primary Pain Types During Treatment
Peripheral Neuropathy Back Pain
This presents as sharp, stabbing pain radiating down your legs following nerve pathways. You’ll notice tingling or weakness that makes standing difficult. Unlike muscle pain, this worsens at night and may feel like “pins and needles” even when resting.
Taxane Acute Pain Syndrome (TAPS)
TAPS strikes 70% of taxane patients within 48 hours of infusion. You’ll experience sharp, burning pain in your hips and lower back that peaks around day 3 before gradually fading—only to return with your next treatment. This differs from peripheral neuropathy because it follows a predictable cycle matching your chemo schedule.
Deep Bone Aches
Some chemo drugs disrupt bone marrow production, creating deep, throbbing pain in your spine and pelvis. This feels like a constant heavy weight that limits your ability to sit upright. Unlike nerve pain, bone aches often improve with movement and worsen with prolonged rest.
Identify Emergency Red Flags Immediately
Spinal Compression Warning Signs
Call your oncology team right now if you experience:
– Sudden leg weakness making stairs difficult
– Loss of bowel or bladder control
– Pain that intensifies when lying flat
– Numbness spreading upward from your feet
These could indicate spinal cord compression—a medical emergency requiring same-day imaging and possible steroid treatment. Don’t wait for your next scheduled appointment.
Infection Indicators During Chemo
Your weakened immunity makes spinal infections dangerous. Seek immediate care if back pain accompanies:
– Fever above 100.4°F
– Redness or warmth along your spine
– Night sweats that soak your pajamas
– Pain worsening when coughing or sneezing
Medication Strategies That Actually Work
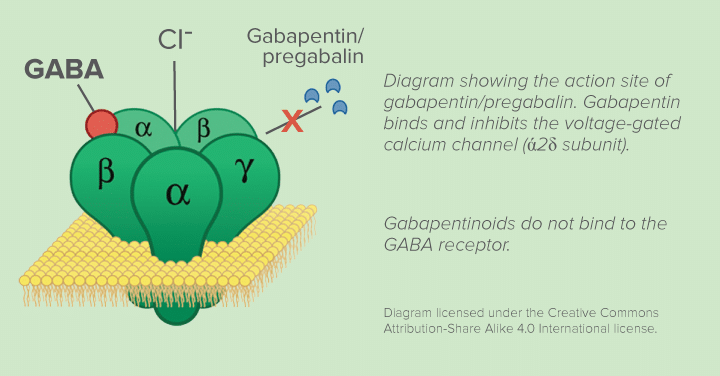
Prescription Solutions for Nerve Pain
Gabapentin and Pregabalin Protocol
Start with 100mg gabapentin at bedtime to minimize drowsiness. Your oncologist will increase by 100mg every 3 days until reaching 300mg three times daily—the effective dose for most patients. Track pain levels daily to determine if pregabalin (Lyrica) at 75mg twice daily works better for your specific nerve pathways.
SNRIs for Dual Benefits
Duloxetine (Cymbalta) at 30mg daily reduces both nerve pain and chemotherapy-related depression. Begin with this lower dose for one week before increasing to 60mg if tolerated. You’ll notice improvement in pain scores within 2-4 weeks as serotonin and norepinephrine levels stabilize.
Safe Over-the-Counter Options
Acetaminophen Protocol
Take 650mg every 8 hours (max 3,900mg daily) for mild muscle aches. Avoid exceeding 3,000mg daily if you have liver concerns. This works best for dull back pain but won’t touch nerve-related burning sensations.
NSAID Precautions
Use ibuprofen 200mg only after confirming with your oncology team. Some chemo regimens like Gemcitabine increase bleeding risk, making NSAIDs dangerous. Never combine with blood thinners without explicit approval.
Critical Warning: Never take new medications—including herbal supplements—without checking with your cancer team. Even “harmless” OTC drugs can interfere with chemotherapy metabolism.
Gentle Movement Exercises That Reduce Pain
Daily Stretching Routine
Morning Spine Mobility Sequence
Complete these before getting out of bed:
1. Knee-to-chest stretch: Hug one knee to chest for 15 seconds (reduces disc pressure)
2. Pelvic tilts: Flatten lower back against mattress 10 times (releases tight muscles)
3. Ankle pumps: Point/flex feet 20 times (improves circulation to prevent blood clots)
Standing Desk Exercises
Every hour, perform:
– Wall angels: Back against wall, slide arms up/down like snow angels (5 reps)
– Seated spinal twists: Gently rotate torso while holding chair (hold 10 seconds/side)
– Heel raises: Lift heels 20 times while holding counter (strengthens calf muscles)
Walking Program That Builds Strength
Week 1-2: Foundation Building
Start with 5-minute indoor walks 3x daily. Focus on posture: shoulders back, chin level. Stop immediately if pain exceeds 4/10 or dizziness occurs. Use a cane if neuropathy affects balance.
Week 3-4: Gradual Progression
Increase to 10-minute walks twice daily. Add gentle outdoor walks on flat surfaces. Track pain patterns—most patients find morning walks cause less discomfort than afternoon walks.
Chair Yoga Poses for Pain Relief
Supported Child’s Pose
Kneel on floor, sit back on heels, rest forehead on stacked hands on chair seat. Hold 1-3 minutes while breathing deeply into your lower back. This decompresses spinal discs without floor strain.
Legs-Up-The-Wall Variation
Lie sideways next to wall, swing legs up until hips touch baseboard. Rest 5-10 minutes. This gentle inversion reduces pressure on lumbar nerves—ideal after long sitting periods.
Heat and Cold Therapy That Targets Pain
:max_bytes(150000):strip_icc()/VWH_Illustration_Contrast-Therapy-in-Physical-Therapy_Danie-Drankwalter_Final-e0dfdcae3d364ff3a5cd87c889684b82.jpg)
Heat Protocol for Muscle Tension
Microwave Heat Pack Method
Fill cotton sock with uncooked rice, microwave 45 seconds. Test on inner wrist before applying to lower back for 15 minutes. The moist heat penetrates deeper than dry heating pads to relax tight muscles.
Shower Therapy
Stand under warm (not hot) water for 7 minutes, directing spray at your lower back. Immediately follow with 5 minutes of wall angels to maintain flexibility gains.
Cold Therapy for Inflammation
Ice Pack Application Schedule
Wrap frozen peas in thin towel, apply to painful area for 10 minutes every 2 hours. Never use directly on skin. This works best within 24 hours of pain flaring—particularly for TAPS-related burning sensations.
Contrast Therapy for Lasting Relief
Alternate 15 minutes heat (warm bath) with 10 minutes cold (ice pack) ending with heat. This “pumping” action reduces inflammation while improving blood flow to damaged nerves.
Nutrition That Supports Nerve and Bone Healing
Anti-Inflammatory Daily Smoothie
Blend for immediate relief:
– 1 cup spinach (vitamin K for bone health)
– ½ cup frozen blueberries (antioxidants)
– 1 tbsp flaxseed (omega-3s reduce inflammation)
– 1 cup fortified almond milk (calcium/vitamin D)
– ½ banana (potassium for muscle function)
Consume within 30 minutes of chemo to maximize nutrient absorption during treatment windows.
Hydration Strategy During Treatment
Aim for 8-10 glasses daily unless fluid-restricted. Add electrolytes if experiencing diarrhea. Dehydration worsens nerve pain—track intake with hourly reminders. Your urine should be pale yellow; dark urine indicates insufficient fluids.
Create Your Daily Pain Management Plan
Morning Routine (12 minutes)
- Take prescribed nerve medication with breakfast
- Complete bed stretches before standing
- Apply heat pack while reviewing daily schedule
- Set realistic activity goals using pain scale
Midday Pain Assessment
Rate pain on 1-10 scale:
– 1-3: Continue light activities with posture checks
– 4-6: Take 5-minute walking break + cold therapy
– 7-10: Rest immediately, contact oncology team if persistent
Evening Wind-Down Protocol
- Perform chair yoga for 10 minutes
- Take Epsom salt bath (1 cup salts) if cleared by doctor
- Journal pain patterns: “Today’s worst pain occurred when…”
- Prepare medications for next morning
Track Your Progress Effectively
Simple Pain Diary Format
Record daily:
– Morning pain level (1-10)
– Activity that triggered worst pain
– Medication effectiveness (1-5 scale)
– Sleep interruptions
– Top relief method
Weekly Review Questions
Ask every Sunday:
– Did pain prevent essential activities this week?
– Which intervention worked best?
– Should I adjust medication timing?
– When to request physical therapy?
Long-Term Recovery Expectations
Realistic Timeline
- During treatment: Focus on symptom management
- 3-6 months post-chemo: Gradual neuropathy improvement
- 6-12 months: Continued recovery with exercise
- 1+ years: Most see significant improvement
Key Insight: Nerve healing occurs at 1mm per day—patience is essential. Consistent gentle movement prevents permanent stiffness.
Communication Strategies With Your Oncology Team
Essential Questions to Ask
- “Is my back pain related to my specific chemo drugs?”
- “Should I see a pain specialist before symptoms worsen?”
- “Are there clinical trials for chemo-induced neuropathy?”
- “When should I worry about spinal complications?”
Appointment Preparation
Bring your pain diary, medication list, and specific examples: “I couldn’t stand long enough to cook dinner Tuesday.” Request physical therapy referrals early—wait times average 3 weeks.
Key Takeaways for Immediate Relief
Your chemotherapy back pain is treatable—not something you must endure silently. Start with heat therapy and the morning spine mobility sequence before considering stronger medications. Track your pain patterns meticulously; this data helps your oncology team adjust treatment. Most importantly, act quickly on red flags like leg weakness or loss of bladder control—these require same-day evaluation.
Remember that relief is possible even during active treatment. What works for others may not help you, and that’s normal. Begin with just two interventions: the 5-minute morning stretch routine and your anti-inflammatory smoothie. Consistency matters more than intensity—small daily actions build significant pain reduction over weeks. You’re not just managing symptoms; you’re actively protecting your mobility and quality of life during this critical treatment phase.

