Your spine locks like a rusted hinge when you bend to grab your keys, sending electric shocks down your leg. That relentless ache that turns sitting at your desk into torture or keeps you awake counting ceiling tiles – severe back pain doesn’t just hurt, it steals your life minute by minute. When over-the-counter pills barely dent the agony, you need proven strategies that actually work. How to treat severe back pain effectively starts with understanding your specific situation and taking targeted action within the first critical 72 hours.
This isn’t about quick fixes or miracle cures. We’ll cut through the noise with evidence-based interventions that address root causes – from immediate relief tactics you can implement tonight to long-term solutions that prevent recurrence. Most severe cases resolve within 6-12 weeks using conservative methods, but timing and precision matter. Skip the guesswork and follow this step-by-step roadmap to reclaim your mobility.
Pinpoint Your Exact Pain Source Before Acting
Why Acute and Chronic Pain Demand Different Approaches
Acute severe back pain hits suddenly – like when lifting a suitcase and feeling immediate tearing in your lower back. This type typically resolves within 4 weeks as inflammation subsides. Chronic severe pain persists beyond 12 weeks, often involving nerve sensitization where even light pressure triggers agony. Critical distinction: Acute pain needs inflammation control, while chronic pain requires nervous system retraining alongside structural treatment.
Spot the red flags requiring ER visits immediately:
– Bowel or bladder control loss (cauda equina syndrome)
– Numbness in groin or inner thighs
– Fever combined with back pain
– Unexplained weight loss with progressive pain
Common Culprits Behind Debilitating Symptoms
Most severe cases stem from mechanical issues rather than emergencies. A herniated disc compresses nerves causing sharp, radiating leg pain that worsens when sitting. Spinal stenosis creates cramping leg pain when walking that eases when leaning forward – like pushing a shopping cart. Key visual clue: If pain shoots below your knee when straightening your leg while lying down (positive straight-leg test), nerve involvement is likely.
Stop the Pain Cycle in the First 72 Hours

The Ice-and-Heat Switch Protocol That Works
Apply cold therapy for 15-20 minutes every 2-3 hours during the first 48 hours to reduce inflammation. Wrap ice packs in a thin towel to prevent skin damage – never apply directly. After 48 hours, switch to moist heat for 20-minute sessions to relax spasming muscles. Pro tip: Freeze a paper cup of water, peel the top, and massage the area in circular motions – this combines cold therapy with gentle movement.
Sleep Modifications for Immediate Relief Tonight
Sleeping on your stomach flattens your spine’s natural curve, worsening pain. Instead:
– Side sleepers: Place a firm pillow between your knees to align hips
– Back sleepers: Bend knees over a pillow to maintain lumbar curve
– All sleepers: Use a medium-firm mattress – too soft increases spinal strain by 30%
Critical mistake: Avoid complete bed rest. Gentle movement every 2 hours prevents muscle weakening that prolongs recovery.
Medication Strategies That Target Severe Pain
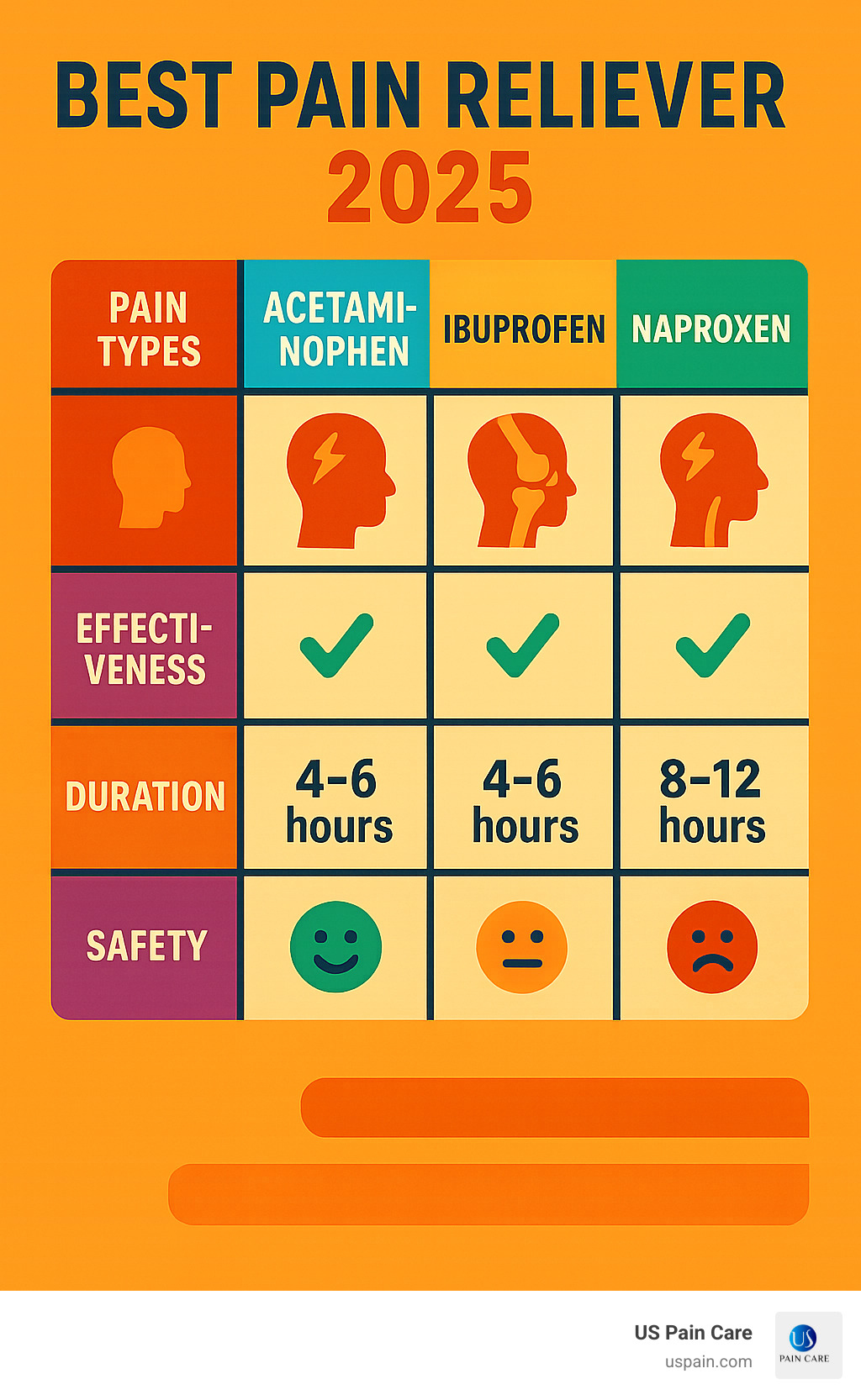
OTC Medications Used Correctly
Start with naproxen (220mg every 8-12 hours) – its longer half-life provides sustained anti-inflammatory effects compared to ibuprofen. Always take with food to prevent stomach bleeding. For nerve-related burning pain, combine acetaminophen (500-1000mg every 6 hours) with topical lidocaine patches applied directly over painful areas. Stop immediately if you notice dark stools or stomach pain – these signal dangerous GI bleeding.
When Muscle Relaxants Become Essential
If OTC options fail after 72 hours, prescription muscle relaxants like cyclobenzaprine (5-10mg at bedtime) can break the pain-spasm cycle. Crucial timing: Take these only at night due to drowsiness – never before driving. Limit use to 2-3 weeks maximum to avoid dependency. For radiating leg pain, gabapentin (300mg nightly, increasing slowly) often works better than opioids with fewer risks.
Physical Therapy Moves That Heal Faster
Core Stabilization Exercises for Severe Pain
Skip traditional crunches that strain your spine. Instead:
– Dead bug: Lie on back, knees bent 90 degrees. Slowly lower one foot to tap floor while keeping lower back pressed down (10 reps/side)
– Pelvic tilts: Flatten lower back against floor by tightening abs (hold 5 seconds, 15 reps)
– Supported bird-dog: On hands and knees, extend opposite arm/leg while keeping hips level (8 reps/side)
Visual cue: Stop if you feel pain radiating – these should create gentle muscle engagement only.
Nerve Gliding Techniques for Radiating Pain
If pain shoots down your leg, perform sciatic nerve flossing:
1. Sit tall in a chair
2. Extend one leg straight with heel on floor
3. Point and flex your foot 10 times while gently nodding chin toward chest
4. Repeat 3x daily
This gently mobilizes trapped nerves without aggravating inflammation.
Professional Treatments That Deliver Results
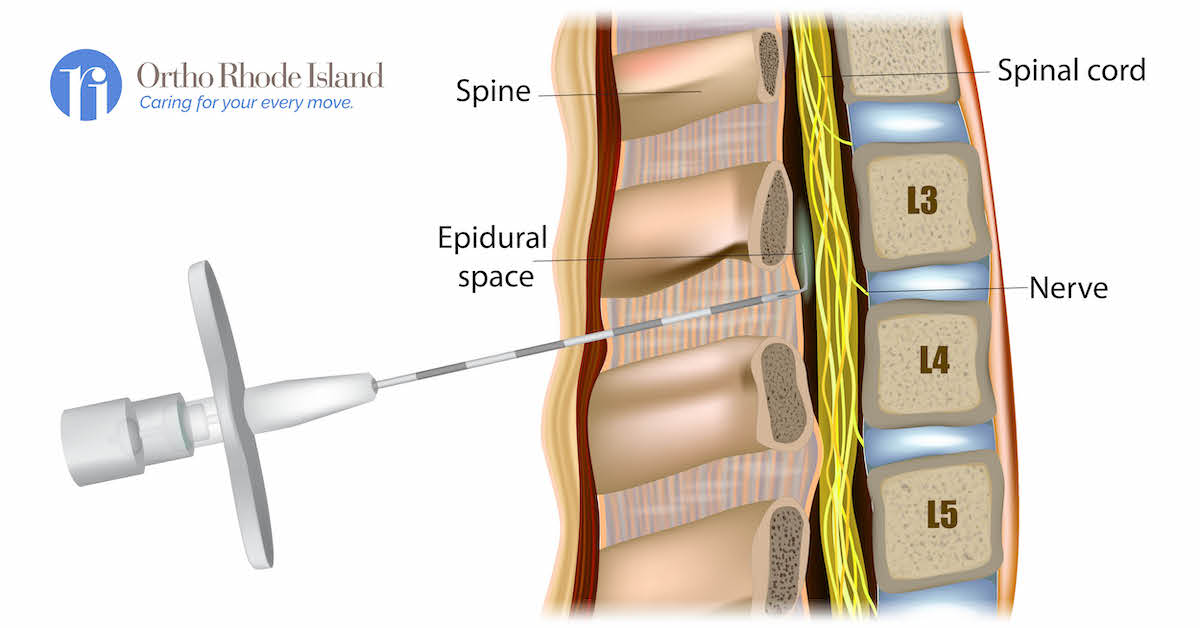
Injection Options Worth Considering
Epidural steroid injections deliver anti-inflammatory medication directly to irritated nerves under X-ray guidance. Realistic expectation: They provide 4-12 weeks of significant relief in 50-75% of patients, buying crucial time for physical therapy. Facet joint injections target arthritic spinal joints – if they provide >50% pain reduction for 3+ months, radiofrequency ablation (nerve zapping) offers 6-12 months of relief.
Physical Therapy Techniques Most Patients Miss
Skilled therapists use directional preference exercises – specific movements that centralize pain (pull radiating symptoms toward your spine). For disc-related pain, repeated backward bending often provides immediate relief. Ask your therapist: “What single movement makes my symptoms better?” – then do it hourly during flares.
Lifestyle Fixes That Prevent Relapse
The 30-Minute Sitting Rule That Saves Your Back
Set phone alarms every 30 minutes when working. Stand up and:
– Perform 3 pelvic tilts against a wall
– Do 10 overhead reaches (arms like a cactus)
– Take 20 steps walking tall
This prevents the cumulative strain that triggers severe episodes. Critical setup: Position your monitor at eye level – looking down 15 degrees increases cervical spine load by 27 pounds.
Lifting Mechanics That Actually Protect You
Forget “bend your knees.” The hip hinge is superior:
1. Stand close to the object
2. Push hips back like closing a car door
3. Keep spine neutral (imagine a ruler along your back)
4. Lift using leg drive while keeping object against your body
Visual check: Your chest should stay up throughout – no rounded shoulders.
Red Flags Requiring Same-Day Medical Attention
Emergency Symptoms You Can’t Ignore
Seek immediate care if you experience:
– Saddle anesthesia: Numbness in inner thighs/groin like sitting on a saddle
– Progressive leg weakness: Difficulty lifting feet while walking
– Bladder changes: Hesitancy or loss of control with back pain
– Night pain that worsens: Especially with unexplained weight loss
These signal potential spinal cord compression requiring same-day imaging.
Build Your Personalized Recovery Plan
The 4-Week Pain Tracking System
Use a simple notebook to log:
– Morning pain score (1-10) before moving
– Activities that worsened pain (e.g., “bent to put on socks”)
– Relief strategies that worked (e.g., “10 min heat + pelvic tilts”)
Pattern recognition: If pain consistently improves with backward bending, focus on extension exercises.
Progressive Exercise Timeline for Full Recovery
- Week 1-2: 5-minute walks hourly, nerve glides, pelvic tilts
- Week 3-4: Add dead bugs (2 sets of 10), hamstring stretches
- Week 5-8: Introduce walking lunges, cat-cow stretches
- Week 9+: Gradual return to gym with therapist guidance
Warning: Pushing too hard before Week 3 often triggers setbacks – respect tissue healing timelines.
Severe back pain demands precision, not patience. By identifying your specific pain generator within 72 hours and implementing targeted strategies – from the ice-heat switch protocol to nerve gliding techniques – you interrupt the pain cycle before it becomes chronic. Most patients achieve 70%+ improvement within 6 weeks using these evidence-based approaches, avoiding unnecessary procedures. Remember: Consistent micro-movements beat occasional intense exercise, and proper lifting mechanics prevent 80% of recurrences. Your path to pain-free living starts with the next movement you make – hinge from your hips, not your spine. Keep this guide handy for your next flare-up, and share it with anyone whose life is limited by back pain.

