Four out of five adults will experience lower back pain at some point, making it one of the most common health complaints worldwide. The good news? Nearly 90% of cases resolve naturally within 12 weeks when you follow proper lower back pain self-care protocols. Whether your pain stems from lifting groceries, sleeping awkwardly, or an intense workout, this evidence-based guide will walk you through proven strategies to reduce pain, restore function, and prevent future episodes. You’ll discover exactly when to use ice versus heat, which movements speed healing, and how to distinguish between normal recovery signs and symptoms that warrant medical attention. Let’s transform your back pain from a debilitating condition into a manageable, temporary setback.
Why Your Lower Back Pain Started Without Warning
Most lower back pain appears without obvious cause, frustrating millions who wake up wondering “what did I do?” Understanding why pain develops helps reduce anxiety and guides effective treatment. Your lumbar spine carries your entire upper body weight through just five vertebrae (L1-L5), with shock-absorbing discs between them. When these discs degenerate or supporting muscles weaken, even routine movements like tying shoes can trigger sudden pain.
Common Non-Traumatic Triggers You Can Control
Your back often reacts to accumulated stress rather than single events. Repeated poor lifting mechanics—using your back instead of legs—creates micro-tears in muscles and ligaments. Carrying extra weight strains back muscles and causes uneven spinal stress, while smoking reduces blood flow to discs, slowing natural healing. Simple overuse from unaccustomed activities like weekend gardening can overwhelm unconditioned tissues.
Age-Related Changes That Increase Vulnerability
After age 30, spinal discs gradually lose moisture and flexibility, making them prone to small tears or bulges. Cartilage between spinal joints naturally thins over time, creating bone-on-bone contact during movement. These normal age-related changes don’t necessarily cause pain but make your back more reactive to everyday stresses. Osteoarthritis in spinal joints further reduces flexibility and increases stiffness.
Immediate Pain Relief Protocol (First 72 Hours)

The first 48-72 hours after onset are critical for minimizing inflammation and preventing chronic pain. Your actions during this window significantly impact recovery speed and completeness.
Cold Therapy Application Guide
Apply ice immediately using these exact steps:
– Wrap ice cubes or frozen vegetables in a thin towel
– Place on painful area for 15-20 minutes
– Repeat every 2-3 hours during waking hours
– Continue for first 48 hours maximum
Ice constricts blood vessels to reduce inflammation and numbs pain signals. Never apply ice directly to skin, and stop immediately if you experience increased pain or skin irritation. This lower back pain self-care step is most effective when started within the first hour of pain onset.
Strategic Rest Positioning
Position yourself correctly to reduce pressure on spinal nerves:
– Lie on firm surface (floor or firm mattress)
– Place small pillow under natural lower back curve
– Position another pillow under knees to maintain slight bend
– Limit total bed rest to 1-2 days maximum
Prolonged inactivity weakens supporting muscles and can actually extend recovery time. Get up and walk every 30-60 minutes for just 2-3 minutes, even if uncomfortable. This gentle movement maintains circulation without straining healing tissues.
Heat Therapy Transition Schedule
After 48-72 hours, switch from cold to heat therapy to promote healing blood flow and relax tight muscles. Applying heat too early can increase inflammation and prolong recovery.
Safe Heat Application Methods
Use these techniques once initial inflammation subsides:
– Heating pad: Set to medium, wrap in towel, apply 15 minutes maximum
– Hot water bottle: Fill with warm (not hot) water, test temperature on inner wrist first
– Warm bath: Soak 15-20 minutes with Epsom salts for muscle relaxation
Never fall asleep on a heating pad, and avoid heat if you have diabetes or circulation issues. Heat therapy should feel soothing—not hot enough to cause redness or discomfort.
Gradual Movement Integration
Begin light movement as soon as tolerated:
– Start with 5-10 minute walks around your home
– Increase duration by 2-3 minutes daily
– Stop immediately if pain worsens significantly
– Aim for 3-4 short walks daily rather than one long session
Research shows back pain decreased by 52.5% in patients who performed regular exercises compared to those who remained inactive. Movement stimulates nutrient flow to spinal discs and prevents stiffness.
Daily Movement That Accelerates Healing
Specific exercises reduce pain by strengthening supporting structures without straining healing tissues. The key lies in choosing movements that match your current recovery stage.
Core Strengthening Sequence for Pain Relief
Start with these gentle exercises after acute pain subsides:
Modified Plank
– Begin on hands and knees
– Lower to forearms, keeping back straight
– Hold 15-30 seconds, build to 2 minutes
– Stop if sharp pain occurs
Pelvic Tilts
– Lie on back with knees bent
– Tighten abdominal muscles, flattening back into floor
– Hold 5 seconds, release slowly
– Repeat 10-15 times
These exercises activate the multifidus muscle that stabilizes your spine. Perform them daily for best results.
Flexibility Restoration Stretches
Use a rolled towel to assist gentle stretching:
Knee-to-Chest Stretch
– Lie on back, wrap towel around one thigh
– Gently pull knee toward chest until stretch felt
– Hold 15-30 seconds, switch legs
– Keep opposite leg bent with foot on floor
Cat-Camel Stretch
– Start on hands and knees
– Arch back upward (like cat), then sag downward
– Move slowly through full range
– Repeat 10 times
High-Risk Movements to Avoid During Recovery
During healing, skip these movements that can re-injure tissues:
– Traditional sit-ups and crunches (strain lumbar discs)
– Running or high-impact aerobics (jarring spinal motion)
– Heavy weightlifting (excessive spinal loading)
– Twisting motions like golf swings (shear forces on discs)
– Toe touches with straight legs (overstretches hamstrings)
All-Day Posture Optimization System
How you position your body during routine activities either supports healing or creates new strain. These micro-adjustments significantly reduce spinal pressure.
Sitting Without Spinal Strain
Most people sit incorrectly, increasing disc pressure by 40%. Here’s how to sit safely:
Proper Sitting Protocol
– Limit sitting to 10-15 minute blocks initially
– Place lumbar roll (rolled towel) at natural lower back curve
– Keep both feet flat on floor, knees at 90 degrees
– Position computer screen at eye level
– Stand up and walk briefly every 15 minutes
Standing Posture Correction
Maintain neutral spine while standing:
– Keep head directly over shoulders
– Tuck chin slightly, avoid forward head posture
– Distribute weight evenly on both feet
– Engage core muscles gently
– Shift weight frequently between feet
Safe Lifting Technique for Daily Tasks
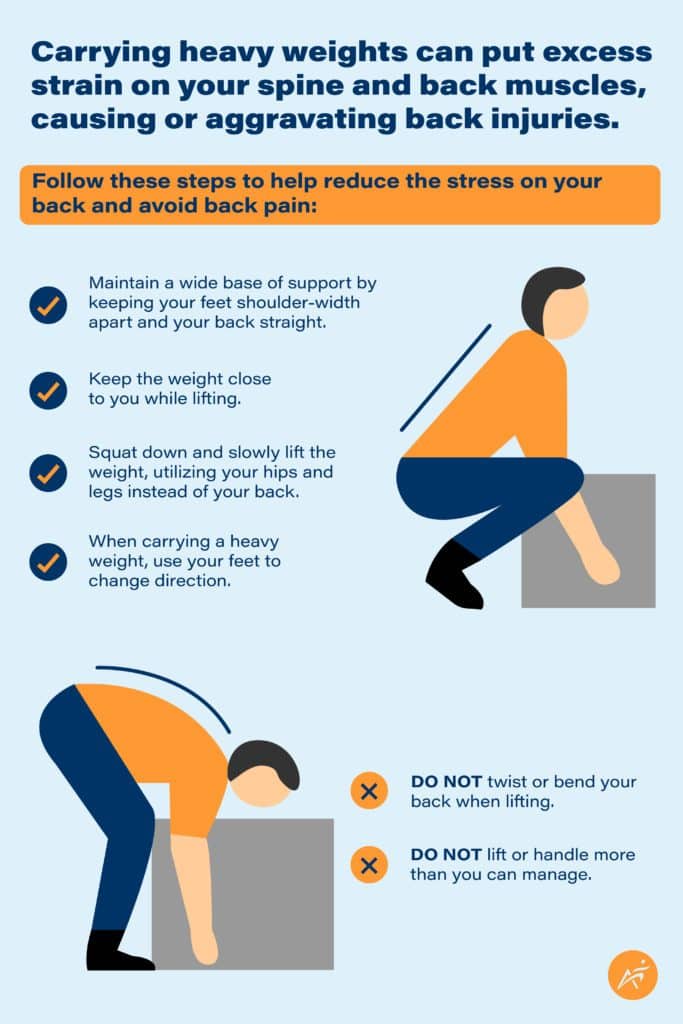
Use the hip hinge technique for any lifting:
– Stand close to object with feet shoulder-width apart
– Bend at hips and knees, not waist
– Keep back straight, chest forward
– Grip object firmly, hold against body
– Lift using leg muscles, not back
– Never twist while lifting—pivot feet instead
– Ask for help with items over 30 pounds
Sleep Position Optimization
Your sleeping posture affects morning stiffness more than most realize.
Side Sleeping Position
– Use firm mattress (place board underneath if too soft)
– Lie on side with knees bent
– Place pillow between knees to align hips
– Hug small pillow to prevent shoulder rolling forward
Back Sleeping Alternative
– Lie on back with pillow under knees
– Place small, rolled towel under lower back
– Use thin pillow under head—avoid neck flexion
– Skip stomach sleeping—it strains neck and back
Anti-Inflammatory Nutrition Protocol
What you eat directly impacts inflammation levels and healing speed. Focus on foods that reduce rather than promote inflammation.
Daily Pain-Reducing Foods
Include these daily:
– Berries: 1 cup mixed berries for antioxidants
– Fatty fish: Salmon or mackerel 2-3 times weekly
– Leafy greens: Spinach and kale in smoothies or salads
– Nuts and seeds: Handful of almonds or walnuts
– Turmeric: Add to meals or take as supplement with black pepper
Inflammation Triggers to Eliminate
Minimize these pain-promoting foods:
– Processed meats and fried foods
– White bread, pasta, and pastries
– Sugary drinks and snacks
– Excessive alcohol
– Foods high in trans fats
Hydration is equally critical—spinal discs are 80% water. Dehydration makes them less effective shock absorbers. Aim for 8-10 glasses daily, more if active or in hot environments.
Medical Red Flags Requiring Immediate Attention
While most back pain resolves with self-care, certain symptoms require professional evaluation.
Emergency Warning Signs
Seek immediate care if you experience:
– Loss of bowel or bladder control
– Numbness in groin area (saddle anesthesia)
– Severe weakness in legs
– Fever with back pain
– Pain following significant trauma
Schedule Healthcare Visit When
Contact your provider if:
– Pain persists beyond 3-4 weeks of consistent self-care
– Pain worsens despite following protocols
– Numbness or tingling extends down legs
– Pain interferes with sleep consistently
– You experience unexplained weight loss
Your 12-Week Recovery Timeline
Understanding typical recovery patterns helps you gauge progress and avoid discouragement.
Week 1-2: Acute Phase
- Focus on pain management and inflammation reduction
- Expect fluctuating pain levels
- Gradually increase walking duration
- Begin gentle stretching when tolerated
Week 3-6: Recovery Phase
- Pain should noticeably decrease
- Start core strengthening exercises
- Return to light daily activities
- Continue posture awareness
Week 7-12: Functional Phase
- Most people achieve 90% recovery
- Resume normal activities gradually
- Maintain exercise routine
- Address any remaining weakness
Long-Term Prevention Habits
Develop these habits to prevent recurrence:
– Daily core exercises: 5-10 minutes of planks and bridges
– Regular stretching: Hamstring and hip flexor stretches
– Posture checks: Set phone reminders throughout day
– Weight management: Maintain healthy BMI to reduce spinal load
– Smoking cessation: Improves disc blood supply and healing
Most people with lower back pain make full functional recoveries within 12 weeks when following these evidence-based lower back pain self-care strategies. Success depends on consistency—perform recommended exercises daily, maintain good posture habits, and listen to your body’s signals. While the path may seem slow, each day of proper self-care brings you closer to pain-free living and builds resilience against future episodes. Remember: your back is designed to heal. These strategies simply create the optimal environment for natural recovery while preventing common mistakes that prolong pain. Start today with the immediate relief steps, then progress gradually through the strengthening and prevention phases for lasting back health.

