If you’ve exhausted conventional treatments for chronic lower back pain yet still struggle with daily discomfort, platelet rich plasma therapy might offer a promising alternative. This innovative approach uses your body’s own healing factors to potentially reduce pain and improve function without surgery or long-term medications. With 60-80% of people experiencing back pain during their lifetime, many are searching for solutions beyond standard care.
Platelet rich plasma injections represent a growing option in the regenerative medicine field, though it’s crucial to understand both the potential benefits and current limitations. While PRP has been used for over three decades in musculoskeletal medicine, its specific application for back pain remains an evolving area with encouraging but preliminary evidence. This guide provides evidence-based insights to help you determine if PRP could be right for your persistent back pain.
Targeted PRP Treatment for Spinal Structures
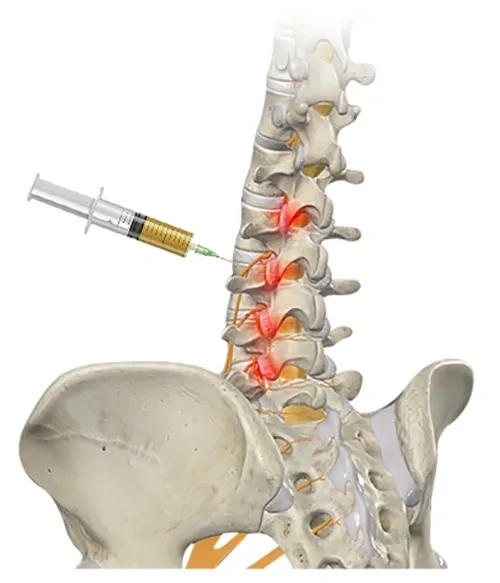
PRP therapy concentrates platelets from your blood into a potent solution containing 3-8 times more platelets than normal blood. These platelets release growth factors like PDGF, TGF-β, and VEGF that may stimulate tissue repair and reduce inflammation in damaged spinal areas. Unlike generic pain treatments, PRP targets specific pain sources with precision.
Direct Delivery to Pain Sources
Your provider can deliver PRP to various spinal structures depending on your specific diagnosis:
– Intradiscal injection: Directly into damaged intervertebral discs causing discogenic pain
– Sacroiliac joint injection: For SI joint dysfunction confirmed through diagnostic testing
– Facet joint injection: Targeting arthritic spinal joints contributing to mechanical pain
– Epidural injection: Around inflamed nerve roots causing radiating symptoms
The growth factors released from activated platelets work gradually to repair damaged tissues, reduce inflammation, and modulate pain signals—addressing both symptoms and underlying causes rather than just masking discomfort.
Evidence-Based Results for Back Pain Relief
Documented Pain Reduction Outcomes
Recent systematic reviews analyzing PRP for back pain show significant improvements across multiple studies involving 127-198 patients between 2018-2023. Patients reported meaningful pain reduction measured by standard scales like VAS and NRS, with one review finding 50% pain relief maintained at three months.
Key effectiveness metrics:
– Pain scores significantly decreased compared to baseline measurements
– One review found PRP more effective than control treatments within 8 weeks
– Oswestry Disability Index scores showed numerical improvements at 3-6 months
– Patient satisfaction rates increased, though detailed measurement tools were limited
Gradual Healing Timeline You Should Expect
Unlike steroid injections that provide immediate but short-term relief, PRP works through a natural healing process:
– Weeks 1-2: Temporary inflammation as healing begins
– Weeks 4-8: Noticeable pain reduction typically emerges
– 3-6 months: Maximum therapeutic benefits become apparent
– 6+ months: Durability varies significantly between patients
This gradual timeline reflects PRP’s regenerative nature rather than simply suppressing symptoms.
Precision Injection Protocols for Maximum Benefit
Standardized Treatment Approach
While protocols vary across clinics, effective PRP treatment follows specific steps:
Preparation phase:
– Blood draw: 30-60ml from peripheral vein
– Processing: 15-20 minutes of centrifugation
– Activation: Calcium chloride or thrombin (method varies by provider)
Injection procedure:
– Imaging guidance: Fluoroscopy or ultrasound for precision
– Injection volume: Typically 2-5ml depending on target area
– Treatment frequency: Single injection versus series (not standardized)
– Procedure duration: Approximately 30-45 minutes total
Condition-Specific Techniques
For discogenic pain:
– Intradiscal injection under fluoroscopic guidance
– Patient positioned prone on procedure table
– Needle advanced through posterolateral approach
– Contrast confirmation before PRP injection
For facet or SI joint pain:
– Ultrasound or X-ray guidance for accuracy
– Small volume injections (1-2ml) targeting specific joints
– Often combined with local anesthetic for comfort
– Requires precise anatomical knowledge for effectiveness
Ideal Candidate Profile for PRP Success
Who Benefits Most from PRP Therapy
Based on current evidence, optimal candidates share these characteristics:
Clinical profile:
– Chronic lower back pain lasting more than 12 weeks
– Failed conservative treatments (physical therapy, medications)
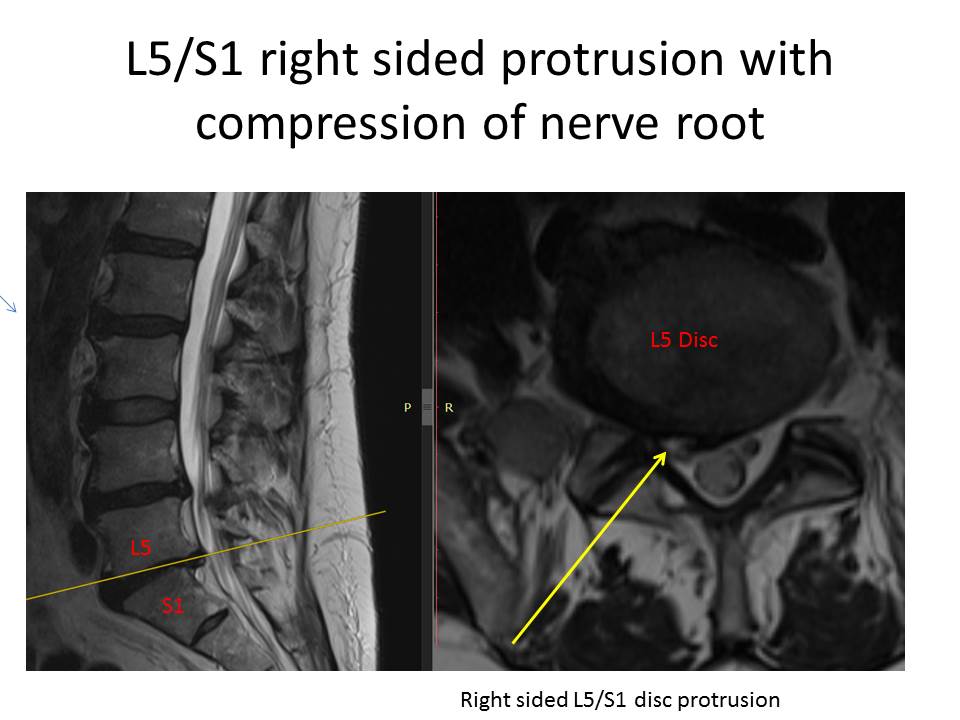
– Discogenic pain confirmed via imaging studies
– Age range 33-53 years (mean from research studies)
– Realistic expectations about gradual improvement
Diagnostic requirements:
– MRI or CT confirming disc degeneration or joint damage
– Positive discography when performed as part of diagnosis
– Absence of red flag symptoms requiring immediate intervention
– No significant spinal instability on imaging
Critical Exclusion Factors to Consider
Absolute contraindications:
– Active infection at injection site or systemic infection
– Known malignancy affecting the spine
– Pregnancy
– Severe coagulation disorders
Relative contraindications:
– Multiple level disc disease without clear pain generator
– Previous spinal fusion at target level
– Active inflammatory arthritis like ankylosing spondylitis
– Current systemic corticosteroid use
Safety Profile: Minimal Risks with Proper Technique
Documented Side Effects and Complications
The current evidence demonstrates PRP’s favorable safety profile across multiple systematic reviews:
Serious complications:
– Zero reports of serious adverse events in any reviewed studies
– No major complications across all research involving 127-198 patients
– Risk profile similar to standard injection procedures
Common temporary side effects:
– Injection site pain lasting 24-48 hours
– Mild muscle soreness around injection area
– Temporary increase in back pain during initial healing phase
– Rare vasovagal response during blood draw or injection
Essential Safety Verification Steps
Pre-procedure verification:
– Thorough screening for contraindications
– Confirmation of appropriate target structure via imaging
– Detailed discussion of realistic expectations
– Comprehensive informed consent process
Post-procedure monitoring:
– Observation period of 15-30 minutes after injection
– Clear instructions for pain management
– Scheduled follow-up at 2-4 weeks
– Guidance on recognizing potential complications
PRP Versus Other Back Pain Treatments
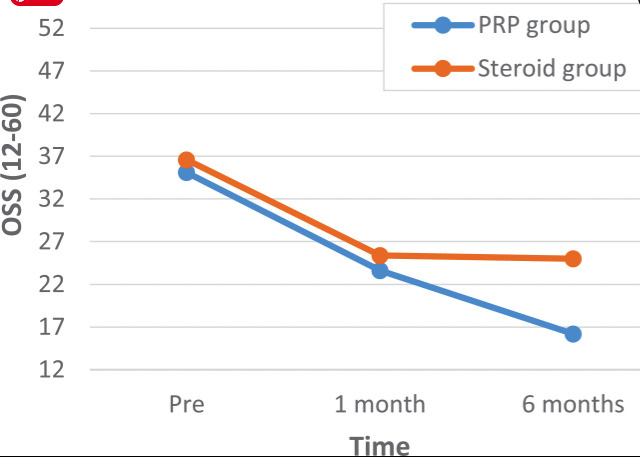
PRP Compared to Steroid Injections
Key comparative advantages:
– Longer-lasting effects (months versus weeks)
– Better patient satisfaction scores
– Addresses underlying tissue damage rather than just inflammation
– Fewer repeat injections needed over time
One systematic review suggests PRP may be superior to steroid injections for pain reduction and patient satisfaction, though more high-quality comparative studies are needed.
Critical Knowledge Gaps in Treatment Comparison
Missing comparative data:
– No studies comparing PRP to physical therapy effectiveness
– Limited evidence versus NSAIDs or other conservative treatments
– Insufficient data on cost-effectiveness compared to standard care
– Research urgently needed across multiple treatment dimensions
This gap makes it difficult to position PRP precisely within standard treatment algorithms.
Realistic Cost Expectations and Access
Financial Considerations
Treatment costs:
– PRP injections typically range from $500-2,000 per treatment
– Multiple injections may be required for optimal results
– Most insurance plans do not currently cover PRP for back pain
– Patients usually pay out-of-pocket for this treatment
Value assessment:
– Compare to ongoing costs of medications or frequent physical therapy
– Factor in potential reduction in work absenteeism
– Consider possible avoidance of more expensive surgical interventions
– Long-term cost-effectiveness remains unclear due to limited data
Availability Challenges
Limited centers offer spinal PRP due to specialized training requirements, regulatory variations by region, and inconsistent quality control standards. This restricted availability makes finding experienced providers crucial for optimal outcomes.
Making Your Informed Decision
Essential Questions for Your Provider
Before proceeding with PRP treatment, ask these critical questions:
– What is my specific diagnosis and how might PRP help my particular condition?
– What are realistic expectations for pain relief and functional improvement?
– How many treatments might I need and what will the total cost be?
– What alternatives exist if PRP doesn’t provide adequate relief?
– How will treatment response be measured and monitored over time?
Decision Framework for Success
Consider PRP when:
– Conservative treatments have failed after appropriate duration
– You’re seeking alternatives to surgical intervention
– You understand the evidence limitations and research gaps
– Cost fits within your budget as an out-of-pocket expense
– You have access to providers with specific spinal PRP experience
Ensure you’ve explored alternatives first:
– Completed a thorough physical therapy program
– Optimized medications under professional guidance
– Considered other injection options appropriate for your condition
– Addressed contributing lifestyle factors like posture and ergonomics
– Obtained second opinions when appropriate for your situation
Final Consideration: PRP represents a promising regenerative option for chronic back pain when standard treatments have failed, but it remains an evolving therapy with significant research gaps. Current evidence suggests meaningful benefits for carefully selected patients with discogenic pain, yet the therapy lacks the robust evidence base of more established treatments. Success depends heavily on proper patient selection, precise injection technique guided by imaging, and realistic expectations about the gradual healing process. Consult with a spine specialist experienced in PRP therapy to determine if this innovative approach aligns with your specific back pain condition and treatment goals.

