That persistent ache has transformed from a minor nuisance into a daily battle, and you’re tired of masking symptoms with painkillers that barely touch the problem. When your doctor suggests injections as the next step for your back pain, confusion often follows—epidural, facet, trigger point… these terms sound like medical alphabet soup rather than solutions. Understanding the specific types of injections for back pain isn’t just clinical jargon; it’s your roadmap to targeted relief that addresses your unique pain source instead of applying generic treatments that might miss the mark entirely.
The frustration of unexplained back pain becomes even more maddening when treatments don’t match your specific condition. Back pain injections aren’t one-size-fits-all solutions—they’re precision tools designed to target particular pain generators with remarkable accuracy. Whether your discomfort stems from compressed nerves, arthritic joints, or stubborn muscle knots, specific types of injections for back pain deliver medication exactly where it’s needed most. By the end of this guide, you’ll confidently recognize which injection targets your specific pain pattern and what questions to ask your doctor for optimal results.
Stop Radiating Nerve Pain with Targeted Epidural Injections
Pinpointing Your Exact Nerve Culprit
When back pain shoots down your leg or arm like an electric shock, epidural injections deliver relief directly to inflamed nerve roots. These procedures target the epidural space—the critical zone just outside your spinal cord’s protective membrane where nerve compression occurs. By placing anti-inflammatory corticosteroids precisely where nerves exit the spine, this approach reduces swelling that squeezes nerve tissue, effectively stopping that shooting pain at its source.
Why Diagnostic Injections Come First
Your pain management specialist might start with a diagnostic epidural containing only anesthetic. If this brings immediate, significant relief, it confirms which specific nerve root is causing your symptoms. Without this crucial diagnostic step, you might receive therapeutic injections that miss the actual pain generator. Therapeutic versions combine anesthetic with corticosteroids like cortisone, providing longer-lasting inflammation control that typically begins working within 2-7 days.
What Really Happens During the Procedure
Don’t picture a scary needle plunge—fluoroscopic X-ray guidance ensures millimeter-perfect needle placement while you lie comfortably face-down. Most patients feel only pressure as the physician positions the needle near the affected nerve. The entire process takes just 15-30 minutes in an outpatient setting, with minimal recovery time required. You’ll leave with specific instructions for monitoring your pain response over the next week to evaluate effectiveness.
Fix Arthritic Spine Joints with Facet Injections

Targeting Your Spine’s Hidden Hinges
Those small, finger-sized joints connecting each vertebra—called facet joints—become major pain sources when arthritis or injury strikes. Facet joint pain often masquerades as general back discomfort but actually radiates to shoulders, buttocks, or thighs depending on which spinal segment is affected. Unlike nerve pain that shoots down limbs, facet joint pain typically stays localized near the spine but can create widespread discomfort.
The Two-Step Diagnostic Process That Works
Accurate diagnosis requires one of two approaches: either injecting anesthetic directly into the suspicious facet joint or targeting the medial branch nerves that carry pain signals from the joint. If either method brings significant pain relief, it confirms facet joint involvement as your primary pain source. This precision matters because treating the wrong structure wastes time and delays real relief.
Long-Term Relief Beyond Steroid Shots
Once diagnosis is confirmed, therapeutic steroid injections provide extended pain control. For stubborn cases, radiofrequency ablation offers months of relief by carefully heating and temporarily disabling the sensory nerves serving the joint. This advanced technique doesn’t damage motor nerves, preserving movement while interrupting only pain signals—a game-changer for chronic facet joint sufferers.
Stop One-Sided SI Joint Pain with Targeted Injections
Recognizing Your SI Joint Pain Pattern
Sacroiliac (SI) joint dysfunction creates a distinctive pain signature—usually one-sided low back, buttock, and upper leg pain that worsens with sitting, standing up, or climbing stairs. Unlike other spinal conditions, true SI joint pain rarely affects both sides simultaneously. If your pain follows this pattern and hasn’t responded to physical therapy, SI joint injections could be your missing solution.
Why X-Ray Guidance Is Non-Negotiable
The gold standard for diagnosing SI joint pain involves X-ray guided anesthetic injection directly into the joint space. Without imaging guidance, accuracy drops dramatically since these joints sit deep within the pelvis. When performed correctly, effective injections should substantially reduce your specific pain pattern within minutes, confirming SI joint involvement with near certainty.
Combining Immediate and Extended Relief
Diagnostic injections use pure anesthetic to confirm the pain source, while therapeutic versions add corticosteroids for longer-lasting benefits. Most patients notice improved sitting tolerance and walking ability within days, with peak effects appearing after 1-2 weeks. For best results, pair these injections with targeted core strengthening exercises that stabilize the pelvis.
Eliminate Muscle Knots with Trigger Point Injections
When Muscle Tightness Becomes Chronic Pain
Those stubborn muscle knots—called trigger points—create referred pain that travels far from their origin, mimicking nerve or joint issues. If you have fibromyalgia, tension headaches, or myofascial pain syndrome, trigger point injections deliver immediate muscle relaxation where it’s needed most. Unlike spinal injections, these target peripheral muscles rather than the spine itself.
The Simple, Quick Procedure You Can Resume Immediately
During this 5-10 minute procedure, your doctor identifies tight, tender muscle bands and injects local anesthetic directly into the knot. Some practitioners add corticosteroids for longer effects, while physical therapists often use “dry needling”—inserting the needle without medication. Best of all, you can drive yourself home and return to normal activities immediately with no downtime.
Why Multiple Sessions Often Work Best
Widespread trigger points typically require several injection sessions spaced weeks apart. Your provider might combine this with manual therapy and stretching techniques to prevent knots from reforming. Patients commonly report immediate relief as the muscle releases its grip, though full benefits build over subsequent treatments as surrounding muscles rebalance.
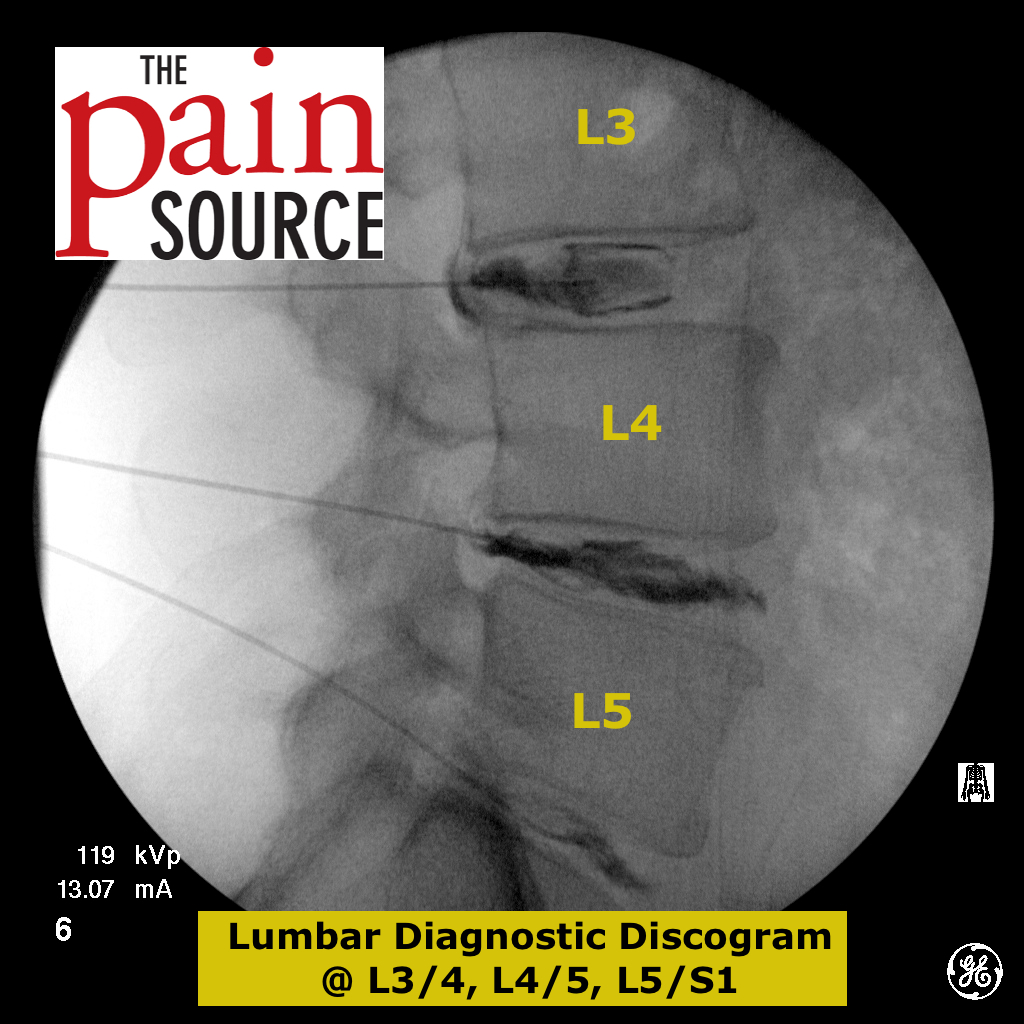
When Discography Pinpoints Surgical Candidates
Why This Diagnostic Test Feels Different
Provocation discography serves one critical purpose: identifying which spinal discs generate chronic, treatment-resistant pain. Unlike other injections that provide relief, discography temporarily reproduces your pain by pressurizing suspect discs with contrast dye. You’ll stay awake during the procedure to provide real-time feedback—when injection recreates your exact pain pattern, that disc is confirmed as your pain generator.
The Role in Surgical Decision-Making
Performed only when surgery is under serious consideration, discography prevents unnecessary operations by confirming which disc levels actually cause pain. Without this precise diagnostic tool, surgeons might operate on the wrong spinal segment, wasting recovery time and potentially worsening symptoms. The procedure’s value lies entirely in its diagnostic accuracy, not pain relief.
What to Expect During the Procedure
Your doctor will inject contrast dye into suspect discs while monitoring your pain response. Significant pressure during injection is normal, but the critical moment comes when it reproduces your typical pain. This information guides whether surgery targets one or multiple disc levels, making it an invaluable tool for complex cases where imaging alone can’t pinpoint the pain source.
Essential Safety Practices for All Back Pain Injections
Why Fluoroscopy Is Your Safety Net
Every legitimate spinal injection uses real-time X-ray guidance (fluoroscopy) to ensure precise needle placement. This imaging confirms the needle reaches the exact target—whether epidural space, facet joint, or SI joint—while avoiding critical structures. Never accept an injection without imaging guidance; accuracy drops dramatically without it, reducing effectiveness and increasing risks.
The Non-Negotiable Exercise Component
Injections alone provide only temporary relief—they’re designed as bridges to structured exercise programs. Your provider should pair injections with specific stretching for spinal mobility and strengthening for stability. Without this crucial component, pain typically returns within weeks as underlying weaknesses remain unaddressed. Think of injections as creating a pain-free window to build lasting strength.
Understanding Real Risks vs. Myths
While complications are rare, potential issues include minor bleeding at the injection site or temporary steroid-related side effects like elevated blood sugar. Serious complications are extremely uncommon when performed by experienced providers using proper imaging. Your doctor will screen for contraindications like blood thinners or infections before proceeding—never skip this safety step.
Choosing Your Best Injection Option
Don’t leave your treatment to chance—armed with knowledge of these specific types of injections for back pain, you can have targeted conversations with your pain specialist. Ask exactly which anatomical structure your injection targets and how it fits into your broader rehabilitation plan. The most effective treatment always matches your specific pain generator, not the latest trend or most aggressive option.
Remember that successful pain management combines precise diagnosis with targeted treatment and consistent rehabilitation. Whether your pain stems from nerve compression, joint arthritis, or muscle dysfunction, the right injection type delivers medication exactly where it works best—giving you the relief needed to rebuild strength and reclaim your active life. Your path to lasting back pain relief starts with understanding which of these seven injection types solves your specific problem.